Welke ooglaser behandelingsmethode past het best bij?
Ooglaseren behelst de behandeling van alle refractiestoornissen zoals bijziendheid, verziendheid en astigmatisme met de excimerlaser. De ooglaser behandelingsmethode is volledig pijnloos en beide ogen worden steeds in één keer behandeld. Pas na een grondig vooronderzoek zal de oogarts beslissen welke ooglaserbehandeling best past bij uw refractiestoornis.
Waarom ooglaseren?
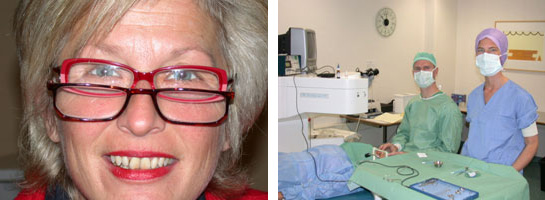
Indien u lenzen draagt kan het zijn dat u lensmoeheid vertoont waarbij u uw lenzen steeds kortere tijd kan verdragen. De oorzaak hiervan is te vinden bij telling van de endotheelcellen met de speculaire microscoop. Een zachte contactlens is als een laagje plastiek op de cornea en zorgt elke dag voor zuurstofgebrek waardoor de endotheelcellen afsterven. Indien de celtelling daalt onder 1200 cellen/mm2 (zie speculaire microscoop) dan treedt er corneaoedeem op waarbij u halo’s ziet en ‘s avonds troebel. Hieronder een plaatje van de endotheelcellen.
Anatomie en functie van de cornea
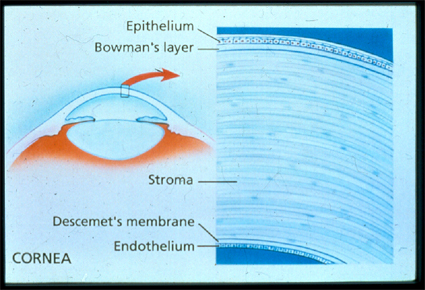 Alle ingrepen gebeuren of op het hoornvlies of op de ooglens. Het hoornvlies is een dun doorzichtig laagje van ongeveer een halve millimeter dik dat zich vooraan het oog bevindt. Het ligt voor de pupil en het regenboogvlies. Achter de pupil ligt de ooglens welke een biconvexe vorm heeft (dus bol) zodat het de binnenkomende lichtstralen juist projecteert op het netvlies achteraan het oog. Alle informatie die toekomt op de gele vlek van het netvlies wordt dan als een electrische impuls via de oogzenuw naar de hersenen doorgestuurd.
Alle ingrepen gebeuren of op het hoornvlies of op de ooglens. Het hoornvlies is een dun doorzichtig laagje van ongeveer een halve millimeter dik dat zich vooraan het oog bevindt. Het ligt voor de pupil en het regenboogvlies. Achter de pupil ligt de ooglens welke een biconvexe vorm heeft (dus bol) zodat het de binnenkomende lichtstralen juist projecteert op het netvlies achteraan het oog. Alle informatie die toekomt op de gele vlek van het netvlies wordt dan als een electrische impuls via de oogzenuw naar de hersenen doorgestuurd.
Types refractiestoornissen
Myopie of bijziendheid: het oog is te lang zodat het licht dat op het hoornvlies valt en gebroken wordt door de cornea en ooglens valt voor het netvlies in plaats van op de gele vlek. Deze patiënten zien niet helder op afstand echter kunnen wel lezen zonder bril of contactlenzen. De laserbehandeling heeft tot doel het hoornvlies af te vlakken zodat de lichtstralen terug op het netvlies geprojecteerd worden.
Hypermetropie of verziendheid: Het oog is te kort zodat de lichtstralen achter het netvlies geprojecteerd worden. De patiënt ziet onscherp voor ver en dichtbij. De laser zal het hoornvlies boller maken zodat de binnenkomende lichtstralen terug scherp op het netvlies vallen.
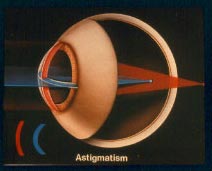 Astigmatisme of cylinderafwijking: Het hoornvlies heeft een verschillende kromming in de horizontale en vertikale as. De vorm is als een rugbybal ipv een ronde bol. De patiënt ziet de lijnen gekromd. De laser zal in de ene as meer corrigeren dan in de andere as zodat de patiënt terug scherp ziet. Deze aandoening komt vaak gecombineerd voor met de hierboven beschreven afwijkingen. De laser zal de verschillende afwijkingen in één stap behandelen. Op dit beeld ziet U dat de vertikale as van de cornea krommer is dan de horizontale.
Astigmatisme of cylinderafwijking: Het hoornvlies heeft een verschillende kromming in de horizontale en vertikale as. De vorm is als een rugbybal ipv een ronde bol. De patiënt ziet de lijnen gekromd. De laser zal in de ene as meer corrigeren dan in de andere as zodat de patiënt terug scherp ziet. Deze aandoening komt vaak gecombineerd voor met de hierboven beschreven afwijkingen. De laser zal de verschillende afwijkingen in één stap behandelen. Op dit beeld ziet U dat de vertikale as van de cornea krommer is dan de horizontale.
Lasik ooglaseren
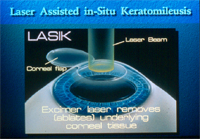 Dit is een ooglasertechniek ter correctie van alle brilcorrecties (van -9 tot +3.5D) . Er wordt een fijn hoornvliesflapje gemaakt op een pijnloze manier. Het ooglaseren duurt enkele seconden en beide ogen kunnen in één tijd behandeld worden. De dag na de laser kan U alle activiteiten hervatten en ziet U reeds erg goed. Indien U ouder bent dan 45 jaar dan zal U na het ooglaseren vaak nog een leesbril nodig hebben tenzij U kiest voor monovision.
Dit is een ooglasertechniek ter correctie van alle brilcorrecties (van -9 tot +3.5D) . Er wordt een fijn hoornvliesflapje gemaakt op een pijnloze manier. Het ooglaseren duurt enkele seconden en beide ogen kunnen in één tijd behandeld worden. De dag na de laser kan U alle activiteiten hervatten en ziet U reeds erg goed. Indien U ouder bent dan 45 jaar dan zal U na het ooglaseren vaak nog een leesbril nodig hebben tenzij U kiest voor monovision.
Lasik ooglaser werd voor het eerst uitgevoerd in 1989 door Dr. Pallikaris uit Griekenland. Het betreft een erg veilige ooglaser techniek met een zeer hoog slaagpercentage. We passen deze techniek toe in 10% der gevallen en in 90% van de gevallen wordt de nieuwe ReLEx SMILE ooglaser techniek toegepast.
ReLEx SMILE ooglaseren
Het maken van een hoornvliesflapje bij ReLEx SMILE ooglaseren is nu overbodig geworden door het gebruik van de “ReLEx SMILE” technologie. De naam staat voor SMall Incision Lenticular Extraction. Deze nieuwe revolutionaire techniek wordt in het BOLC toegepast door Dr. De Wilde. De correctie van myopie en astigmatisme kan nu volledig in “one step” met één laser (de femtosecondlaser) worden uitgevoerd en biedt heel wat voordelen. De techniek geeft minder “droog oog” probleem postoperatief omdat we geen flap meer hoeven te maken. De zenuwen in de cornea worden nog nauwelijks beschadigd. Het is te vergelijken met de evolutie van een open buikingreep naar een sleutelgatoperatie. De stabiliteit, integriteit van het hoornvlies en het nachtzicht zijn beter na de ingreep dan met de klassieke flapjestechniek. Omdat we in een gesloten milieu werken verhoogt ook de precisie.
Lees meer over de ReLEx SMILE ooglaseren via onderstaande link
Custom Lasik
Dit is een ooglasertechniek waarbij we speciale software gebruiken. Er wordt voor deze gepersonaliseerde techniek gekozen door de arts indien het hoornvlies erg dun is of u ‘s nachts een erg wijde pupil hebt en klachten hebt van slecht nachtzicht. Indien na een grondige analyse met de aberrometer er hoge orde aberraties blijken te zijn dan zal de arts eventueel ook beslissen dat Custom lasik voor u de oplossing is. Na de lasertherapie zal u dan beter kunnen zien bij ‘s avonds met de auto rijden en ook zal het contrast verbeteren. U zal ook minder hinder ondervinden van halo’s omheen de voorwerpen. In ongeveer de helft van de gevallen zien we dat de patiënten een of meerdere lijnen winnen bij het lezen van de Snellen kaart. We bekomen dus als het ware “arendsogen”. Het maken van het hoornvliesflapje gebeurt op dezelfde manier als bij Lasik.
PRK
De laserstralen komen op de oppervlakkige epitheellaag terecht. Na de wordt een beschermende contactlens op het oog geplaatst voor een drietal dagen. Het herstel verloopt trager dan bij Lasik en het zicht kom trager terug dan bij Lasik. De arts kan voor PRK kiezen indien het hoornvlies bijvoorbeeld te dun is voor een Lasikbehandeling. Beide ogen kunnen samen behandeld worden. We voeren deze behandeling uit in 15% van de gevallen.
PTK
Therapeutische laserbehandeling voor recidiverende corneaerosie. De laser schaaft een fijn laagje van het membraan van Bowman zodat het openscheuren van het hoornvlies voorkomen wordt. Na de behandeling wordt een contactlens geplaatst. Het zicht herstelt pas na enkele dagen.
Bioptics
Bij deze combinatietechniek van lensimplantatie en laser kan men bijziendheid van meer dan -9 D en verziendheid van meer dan + 4 Dioptrie behandelen. Eerst wordt de lensimplantatie uitgevoerd onder druppelnarcose van het ene oog. Deze lens welke U ziet op de afbeelding klikt met 2 klauwtjes vast op het regenboogvlies. Het tweede oog wordt in principe een week later geopereerd. De lasercorrectie met Lasik van de restrefractie gebeurt dan 6 weken later in één tijd aan beide ogen.
We implanteren meestal de ICL-implantlens, wat een heel dunne plooibare lens is welke postvat net voor het voorkapsel van de eigen lens, dus zich achter de pupil bevindt. Deze lens bezit geen klauwtjes en steunt op de zonulavezels van de eigen lens. Ze kan gebruikt worden voor de correctie van hoge myopie of forse hypermetropie. We dienen geen hechting te plaatsen. Nadien kan de eventuele restrefractie worden opgelost met een Lasik behandeling. 1 à 3% der patiënten kan op termijn wel cataract ontwikkelen. De procedure is echter reversibel.Deze lens biedt ook de oplossing bij de behandeling van keratoconus wat betreft de myopiecomponent.We beschikken over de Vumax echografie apparatuur waarmede we heel precies de oogstructuren in beeld kunnen brengen en alzo steeds op een betrouwbare manier de lensdiameter kunnen bepalen.Er worden nu ook torische ICL geïmplanteerd waarbij zowel de myopie als de cylinderafwijking van het oog worden gecorrigeerd.
Corneatransplantatie
Door het troebel worden van het hoornvlies kan het zicht dermate mistig worden dat uw oogarts beslist om het hoornvlies te vervangen. Het hoornvlies is afkomstig van een corneabank en betreft een hoornvlies van een pas overleden persoon. Er kunnen verschillende redenen bestaan waarom een hoornvlies troebel wordt. Meest frequent gaat het om een keratoconus, een aangeboren aandoening waarbij het hoornvlies in één sector verdunt en daardoor een erg stijle kromming gaat vertonen. Door het uitvoeren van een hoornvliestopografie stelt de oogarts de aandoening vast. Andere redenen van een troebel hoornvlies kunnen zijn:
- verlies van endotheelcellen jaren na cataractoperatie met voorkamerlensimplant.
- corneadystrofie.
De operatie gaat door onder algemene narcose en duurt ongeveer één uur. Het principe is dat we met een trepaan het zieke hoornvlies verwijderen en dan het nieuwe hoornvlies inhechten, zodat het zicht terug helder wordt. Het herstel verloopt over ongeveer 1 maand. U dient het oog 6x per dag te druppelen met cortisone om afstoting van de ent te verkomen. U dient ook een vochtinbrengende ooggel toe te dienen.
Nevenwerkingen op korte termijn
De meest frequente nevenwerking is dat er eventueel nog een bijcorrectie dient te worden uitgevoerd omdat na de eerste ooglaser therapie we nog geen optimaal resultaat konden bekomen. Dit gebeurt een tweetal maand na de initiële ooglaser behandeling en komt voor in 5 % van de gevallen. De kans op infectie is minimaal (1/3000) omdat de gelaserde zone wordt beschermd door een flapje.
Na de laser dient U antibiotische druppels in te brengen welke een infectie voorkomen. Indien er toch een infectie optreedt dan zal Uw oog rood worden en het zicht verminderen. U dient dan dringend contact op te nemen met de praktijk voor speciefieke behandeling. Na de ingreep kan ook inflammatie optreden van de flap.
Dit komt voor in 1/400 en wordt behandeld met cortisone druppels. Soms wordt onder de flap gespoeld om een eventueel pluisje te verwijderen.Het maken van de flap kan ook gepaard gaan met eventuele complicaties. Zo kan de flap niet perfect gecentreerd zijn of kan door technisch falen van de keratoom, welke de flap maakt, de flap voorbeeld onvolledig zijn. In dit geval moeten we een zestal weken wachten alvorens de procedure te kunnen hervatten. Hieronder een afbeelding van de keratoom waarmede we het hoornvlies flapje maken.
Patiënten kunnen ook hinder ondervinden van halo’s, of een storende ring rond een lichtbron. In de regel zal dit neveneffect na enkele maanden verdwijnen. Epitheelingroei is een afwijking welke vooral optreedt nadat we een bijcorrectie hebben uitgevoerd. Er groeien celletjes onder de flap welke we naderhand dienen weg te spoelen.
Nevenwerking op middel-en lange termijn
Als late complicatie kan een corneaectasie optreden. Er onstaat van binnenuit een soort blaasje op de cornea waardoor de visus daalt. Deze afwijking is uiterst zeldzaam en treedt vooral op indien men te diep zou laseren. Dit is initieel te verhelpen met een halfharde contactlens en in tweede fase kunnen we opteren voor een corneal crosslinking (CXL).
Met deze methode wordt het collageen van het hoornvlies verstevigd. De indicatie is vooral evolutieve keratoconus echter ook marginale pellucide degeneratie, cornea-ectasie en na PRK. Er wordt eerst een kleurstof (riboflavine) op de cornea gebracht. Daarna wordt het hoornvlies met UV led licht bestraald gedurende 30 minuten om deze kleurstof te activeren. Alzo neemt de rigiditeit van het hoornvlies met 300% toe.
De frequentie van complicaties is vooral afhankelijk van de ervaring welke de chirurg heeft. Lasik wordt in het BOLC reeds sinds 1997 uitgevoerd en er is dus reeds een zeer brede ervaring met deze techniek. Dr. De Wilde voerde zelf reeds meer dan 5000 lasik ingrepen met succes uit. Lasik kan ook worden toegepast indien na een corneatransplantatie er nog een restcorrectie overblijft of indien na de PRK het resultaat niet optimaal is of indien er na een cataractoperatie nog een groot refractieverschil blijft bestaan tussen de beide ogen.